Introduction
Long-term polyphasic sleeping seems like a dream with all the sleep reduction one would get, but its metabolic effects would deserve special attention. Short-term polyphasic sleeping has been natural and viable to a lot of extents; however, on the scale of long-term exposure, such as 1 decade and longer, it could spell a very different vision.
Since there has been no longitudinal or meta-analysis polyphasic study in existence, it is impossible to judge. Specifically, no resources or studies anywhere have shown how polyphasic sleeping fares in the long run. This includes reducing biphasic schedules and the necessary metabolic effect criteria. Therefore, this post will lean towards certain speculations and implications for perpetual polyphasic sleep practice.
Hopefully in the future, there will be dedicated research on this matter to elucidate polyphasic sleeping’s mechanisms.
Generic Metabolic Effects & Sleep
Several studies have demonstrated how chronic sleep deprivation, or even partial sleep deprivation can threaten metabolism. However, the outstanding issue is that these studies focus on shortened monophasic sleep; most studies do not even allow naps.
The most glaring metabolic problems include the following:
- Increased hunger and appetite1
- Obesity2
- Type 2 diabetes1,2
- Increased mortality3
The lacking evidence for polyphasic sleep is astounding, aside from the appearance that “polyphasic sleep gives less sleep so it is the same thing”. In fact, this has been a go-to quote for a lot of polyphasic skeptics. However, it is worth noting the following in all of the cited studies:
- They never mentioned how important NREM2 is regarding metabolism. This includes the minimum required NREM2 duration each day. NREM2 is an important determinant because most polyphasic schedules reduce a certain amount of NREM2 duration.
- The participants in these studies often have sleep issues; this suggests that they are potentially not meeting their daily REM and SWS requirements with shortened monophasic sleep. Thus, sleep quality may be the deciding factor, not sleep duration.
- The potentially inconsistent/random sleep times, meal times and not following the dark period before sleep may also play some roles in these health problems.
Extreme Polyphasic Schedules
It appears that even after a successful adaptation, there are likely long-term metabolic effects of polyphasic sleeping. These effects seem even more apparent on extreme schedules. There is plenty of evidence to support this; additionally, the consensus from veterans on extreme schedules seems to be the enhanced hunger.
A case of this is Aeia, who reportedly lived on Uberman between June 2009 and March 2010.
- She also logged her experience on her YouTube channel.
- However, she eventually quit because she was gaining weight regardless of diets.
- Her story coincides with research linking increased risk of obesity to nighttime eating on regular sleep schedules4; as a result, it may suggest that polyphasic sleep is no different in this aspect.
Other Implications
Although not entirely relevant, there has been research on animals who live under an extreme nap-only regime.
- Given such massive amounts of wake time, such animals, however, spend a lot of their wake time foraging food. If they do not get to eat for a certain amount of time, they would die5.
- Obviously, we cannot extrapolate this information and apply it to humans; it is merely some thoughts because it seems to coincide with Aeia, who likely has eaten around the clock on Uberman.
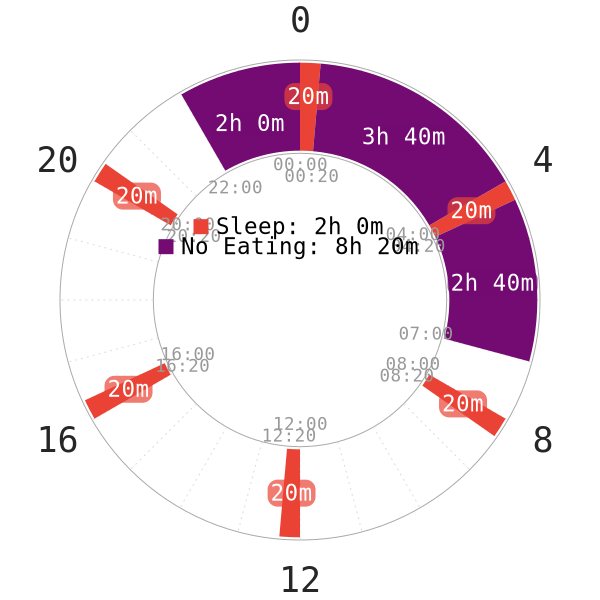
Fasting & Metabolism
Whether keeping an intermittent fast during the night period would completely mitigate this issue is unclear; however, reducing nighttime eating could significantly help obese people.
- The energy from food intake can often counter sleepiness that may otherwise occur from having low volumes of sleep. This process may require a diet based on energy sources with slower release (protein and low GI food). Therefore, food that contain complex carbohydrates and a lot of fiber are good candidates.
- There may also have to be an increased in food intake during the adaptation period. This is because it is generally more demanding than maintaining the schedule afterwards.
- Reduced SWS also directly contributes to type 2 diabetes because SWS can regulate glucose levels and maintain its homeostasis. Suppressing SWS as a result reduces insulin sensitivity and glucose tolerance6. This again stresses on the importance of vital sleep stages and well-being.
- Since we are only collecting long-term extreme polyphasic practice so far, we cannot give a concrete evaluation on the remaining polyphasic schedules, barring a well-nourished Biphasic schedule.
Since nap-only schedules cannot cover the necessary SWS requirements in an average human, Aeia’s diary about gaining weight and increased hunger seems to check out. Because of her blatant inability to continue with her Uberman schedule, it raises the question of whether nap-only schedules can be sustainable long-term at all. This at least applies for sleepers with normal SWS requirements.
Main authors: Crimson & GeneralNguyen
Page last updated: 3 February 2021
Reference
- Spiegel, K., Tasali, E., Penev, P., & Cauter, E. V. (2004). Brief Communication: Sleep Curtailment in Healthy Young Men Is Associated with Decreased Leptin Levels, Elevated Ghrelin Levels, and Increased Hunger and Appetite. Annals of Internal Medicine, 141(11), 846. doi:10.7326/0003-4819-141-11-200412070-00008
- Zhu, B., Shi, C., Park, C. G., Zhao, X., & Reutrakul, S. (2019). Effects of sleep restriction on metabolism-related parameters in healthy adults: A comprehensive review and meta-analysis of randomized controlled trials. Sleep Medicine Reviews. doi:10.1016/j.smrv.2019.02.002
- Maurovich-Horvat, E., T. Z. Pollmacher, and K. Sonka. “The effects of sleep and sleep deprivation on metabolic, endocrine and immune parameters.” Prague Med Rep 109.4 (2008): 275-285.
- Ratini M. What Is Night Eating Syndrome? WebMD. https://www.webmd.com/mental-health/eating-disorders/binge-eating-disorder/what-is-night-eating-syndrome. Published 2017. Accessed November 4, 2018.
- Stampi, Claudio. Why We Nap : Evolution, Chronobiology, and Functions of Polyphasic and Ultrashort Sleep. Birkhauser, 2014.
- Tasali, E., Leproult, R., Ehrmann, D. A., & Van Cauter, E. (2008). Slow-wave sleep and the risk of type 2 diabetes in humans. Proceedings of the National Academy of Sciences, 105(3), 1044–1049. doi:10.1073/pnas.0706446105.
