Wake After Sleep Onset (WASO)
Wake after sleep onset (WASO), or interrupted sleep, is a massively popular sleep issue in humans. By definition, it is periods of wakefulness that occur after sleep onset1. Specifically, interrupted sleep is measured in duration (minutes) to reflect on sleep fragmentation. It also directly shows how long it would take for an individual to go back to sleep. Moreover, there can be more than one occasion of interrupted sleep at night.
Most notably, WASO is also a form of insomnia. However, it is the inability or difficulty maintaining sleep, rather than falling asleep. Troubles with falling asleep is sleep onset insomnia instead.
Because of the problematic nature of WASO, it is then necessary to delve into its behavior as well as how polyphasic sleep can improve it.
Causes of Interrupted Sleep
Interrupted sleep is undoubtedly very common in monophasic sleep. This is because many factors, including subtle ones, can disrupt sleep continuity. We present some of the most common causes that contribute to WASOs.
- Cellphone use around bedtime2. This is very common in college students and teenagers.
- Sleep apnea3
- Late stage of pregnancy4
- Age. The elderly naturally has more fragmented sleep5.
- Caffeine6. Even though the thresholds vary between individuals, it is not advisable to consume caffeine on a polyphasic schedule.
- Energy drinks. These are especially problematic for adolescents7.
- Chronic illnesses8.
- Nocturia, or waking up at night to use the bathroom9.
- Snapping out of dreams (e.g, nightmares, traumatic dreams or anxiety dreams10).
Sleep Stage Mechanics
Interrupted sleep degrades sleep quality; how big of an effect depends on how often these interruptions occur and how long it takes you to fall asleep again. Below are some deleterious effects of interrupted sleep on sleep stages.
- If you wake during the night and go back to sleep, the sleep cycle continues where it left off. The end result is the replacement of quality sleep with light sleep as the cycle resumes11.
- WASOs can destroy the stability and continuity of a specific sleep stage (e.g, REM). As a result, it is more common to experience more abrupt transitions between sleep stages as sleep stages are interrupted more often12.
- Interrupted sleep boosts the vulnerability of maintaining NREM2; this means that it is easier for sleepers to drift back to NREM1, a sleep stage with no actual sleep13.
If you schedule two sleep segments too close together, the same thing occurs. Unpredictable cycles will ensue and lead to bad wakes, more shallow sleep and lower compression.
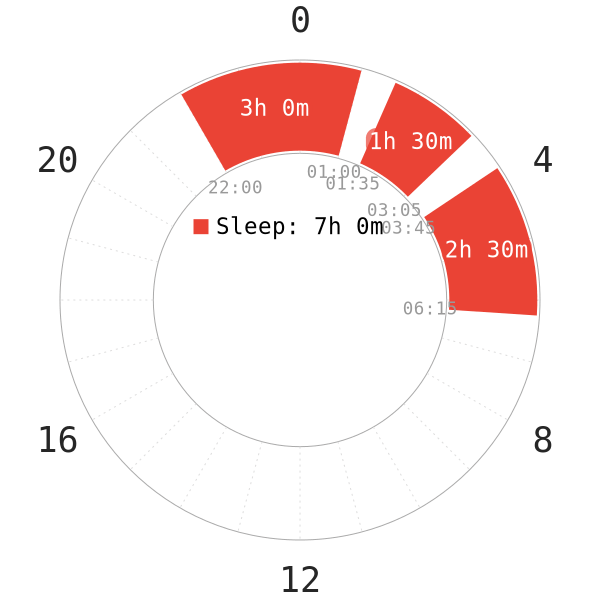
NOTE: Despite that WASO is very disruptive, adults with normal health actually naturally incur some WASO duration in their sleep. This duration is found to be approximately ~30 minutes over a total sleep of ~7 hours14.
These instances usually are negligible and sleepers often are not aware of their “wakefulness” during sleep.
Using Involuntary WASO to your advantage!
If you are waking up every day after a specific amount of time (usually after a whole number of sleep cycles), you may be a naturally segmented sleeper. If you wish to learn more about how you can use this condition to your benefit to adapt to certain schedules easier, you can read more here.
Methods to Combat Interrupted Sleep
Although scientific methods to combat WASOs have not been fully described, there are anecdotally effective means to improve sleep interruptions. Below are some common and working methods.
- Relaxation methods: Yoga, autogenic training and other meditation practices help reduce WASO occurrences and duration.
- Scheduling bigger wake gap between each sleep: You should leave at least 1 BRAC (approx. 2 hours) between sleep segments; however, many people usually enjoy a slightly longer wake duration for more useful activities.
- Anecdotal evidence suggests that 2 or even 3 BRACs would be preferable (3-4 hours).
- Some people have reported great discomfort and a very hard time adapting to wake periods with less than 2 BRACs apart.
- Reducing sleep duration: This is part of the reason why polyphasic sleeping can handle WASOs very well. It is because sleep reduction cuts down on light sleep and increases the time spent in deeper sleep stages.
Polyphasic adaptation
During the adaptation process to a polyphasic schedule, WASOs do occur more often; this is especially the case in later adaptation stages.
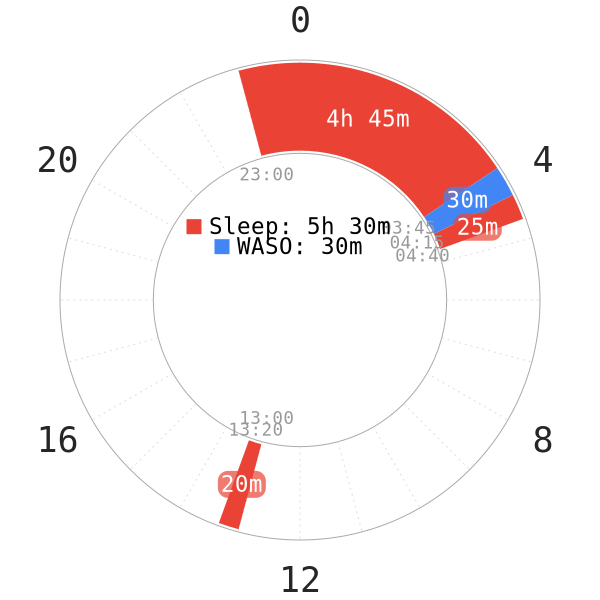
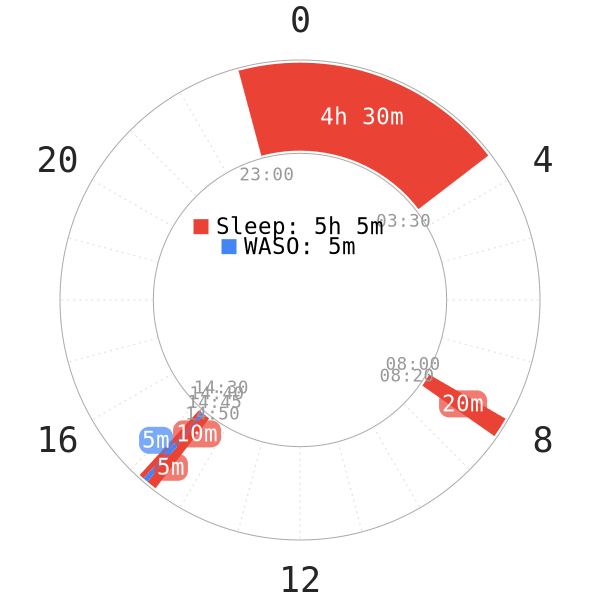
The probable cause for the interruptions is the ongoing sleep stage repartitioning. However, it usually happens mostly in Stage 3 and 4. Thus, the transition between sleep stages may yet to be consistent and smooth. Bursts of NREM2 or emphatic dream contents may wake you up naturally.
The general rules to deal with these WASOs are as follows:
- If you naturally wake up before your scheduled sleep time, get out of bed. This applies to cases where there are less than 5 minutes left of a nap and 30 minutes of a core.
- For example, if your E1 core is supposed to end at 6 AM, and you happen to wake up at 5:30 AM or a bit later but still before 6 AM, get out of bed instead.
- If you try to sleep in, you may wake up during SWS and oversleep.
- Falling back asleep could also be difficult and you would have to spend time trying to do so. It is overall not worth it.
- If there is at least 90 minutes left of a core (1 full cycle), you can try to go back and get as much sleep as possible.
- After adaptation is complete and your overall sleep architecture has been stable, you can go back to sleep the remaining portion of a nap. You are unlikely to oversleep at this point. Furthermore, getting some more sleep can sustain your wakefulness better until the upcoming sleep block. This is really useful if you have to delay your next sleep block a bit.
Main author: GeneralNguyen
Page last updated: 30 March 2021
Reference
- Shrivastava, Deepak, et al. “How to interpret the results of a sleep study.” Journal of community hospital internal medicine perspectives 4.5 (2014): 24983. [PubMed]
- Dowdell, E. B., & Clayton, B. Q. (2018). Interrupted sleep: College students sleeping with technology. Journal of American College Health, 1–7. doi:10.1080/07448481.2018.1499655. [PubMed]
- Cherniack, N. S. “Sleep apnea and its causes.” The Journal of clinical investigation 73.6 (1984): 1501-1506.
- Wilson, Danielle L., et al. “Decreased sleep efficiency, increased wake after sleep onset and increased cortical arousals in late pregnancy.” Australian and New Zealand Journal of Obstetrics and Gynaecology 51.1 (2011): 38-46. [PubMed]
- Ohayon, Maurice M., et al. “Meta-analysis of quantitative sleep parameters from childhood to old age in healthy individuals: developing normative sleep values across the human lifespan.” Sleep 27.7 (2004): 1255-1273. [PubMed]
- Clark, I., & Landolt, H. P. (2017). Coffee, caffeine, and sleep: A systematic review of epidemiological studies and randomized controlled trials. Sleep Medicine Reviews, 31, 70–78. doi:10.1016/j.smrv.2016.01.006. [PubMed]
- Van Batenburg-Eddes, T., Lee, N. C., Weeda, W. D., Krabbendam, L., & Huizinga, M. (2014). The potential adverse effect of energy drinks on executive functions in early adolescence. Frontiers in Psychology, 5. doi:10.3389/fpsyg.2014.00457. [PubMed]
- Meltzer, Lisa J., and Melisa Moore. “Sleep disruptions in parents of children and adolescents with chronic illnesses: prevalence, causes, and consequences.” Journal of pediatric psychology 33.3 (2008): 279-291. [PubMed]
- Ancoli-Israel, Sonia, Donald L. Bliwise, and Jens Peter Nørgaard. “The effect of nocturia on sleep.” Sleep medicine reviews 15.2 (2011): 91-97. [PubMed]
- Inman, D. J., Silver, S. M., & Doghramji, K. (1990). Sleep disturbance in post-traumatic stress disorder: A comparison with non-PTSD insomnia. Journal of Traumatic Stress, 3(3), 429–437. doi:10.1007/bf00974782. [PubMed]
- Aaron J, Carlisle C, Carskadon M, Meyer T, Hill N, Millman R. Environmental noise as a cause of sleep disruption in an intermediate respiratory care unit. Sleep. 1996;19(9):707-710. [PubMed]
- Bianchi, M. T., Cash, S. S., Mietus, J., Peng, C.-K., & Thomas, R. (2010). Obstructive Sleep Apnea Alters Sleep Stage Transition Dynamics. PLoS ONE, 5(6), e11356. doi:10.1371/journal.pone.0011356. [PubMed]
- Wei, Yishul, et al. “Sleep Stage Transition Dynamics Reveal Specific Stage 2 Vulnerability in Insomnia.” SLEEP 40.9 (2017). [PubMed]
- Loredo, J. S., et al. “Sleep quality and blood pressure dipping in normal adults.” SLEEP 27.6 (2004): 1097-103. [PubMed]
