Introduction
Strictness of sleep times is a very important determinant in polyphasic adaptations. It is in your best interest to be as strict as possible with your sleep times, including short naps. This article will detail different mechanics regarding oversleeping and how to optimize adaptation success rate.
Oversleeping and Crashing
Oversleeping Mechanics
In the context of polyphasic sleep, sleeping any time outside any scheduled sleep sessions is known as “oversleeping”, or “crashing”. This includes the following:
- Falling asleep at the wrong time
- Microsleeping for seconds up to several minutes
- Inability to wake up from a nap or core on time.
For example, if the original nap time is at 12:50-13:10, but the sleeper takes it at 13:00-13:20 instead, they both underslept (waking early) and overslept (sleeping early) by 10 mins. Assessing the adaptation setback from oversleeping is difficult, as it depends on several factors.
- Oversleeping duration. The longer it is, the more devastating it becomes.
- The schedule’s total sleep. Usually, a schedule with less sleep will be more negatively affected by oversleeping than a schedule with more total sleep.
- Adaptation progress. The more progress, the more problematic each oversleeping becomes. This is because it is usually easier to start over after only a couple days into an adaptation.
- When and how the oversleep happened. This might also affect the adaptation setback and difficulty.
- Approximately, oversleeping a nap is a setback of one to a few days.
- Having a huge multiple-hour oversleep (over 100-200% of the total scheduled time) can just cause an entire reset.
How Oversleeping Affects Adaptation
Any form of oversleeping is detrimental to adaptation for a lot of reasons and results in big consequences.
- For example, a typical oversleep only partially cures some minor sleep deprivation. Thus, you end up with worse symptoms after proceeding, while the adaptation progress delays.
- Oversleeps interfere with how the body learns the sleep schedule. You will then be tired at the wrong times.
- Oversleeping can easily become habitual. This is the natural response to sleep deprivation by oversleeping/crashing, rather than by adapting. This results in more frequent oversleeping, or Oversleeping Syndrome, OSS.
- It is common to feel great for a few days after an oversleep. This would recover some sleep deprivation, usually 1-5 days. Afterwards, there will be a big energy crash with new energy lows. However, this feeling usually subsides after about a week because the usual sleep deprivation symptoms replace it.
- In addition, the increase in total sleep time leads to a reduction in sleep quality and an extension of cycle length. This contrasts with the compressed sleep quality that is essential in polyphasic sleep.
- Most importantly, a common response to oversleeping is the loss of the temporary napping ability or getting REM naps. Ultimately, this deficit further boosts the risk of oversleeping due to exhaustion.
Oversleeping and Perpetual Sleep Deprivation
All in all, you should learn from each oversleep and make changes to prevent future oversleeps. Getting stuck in OSS every few days would eventually shut down adaptations due to severe sleep deprivation. Long-term sleep deprivation leads to the following:
- Holistic symptoms: Obesity1, diabetes2, increased heart rate3, headaches4, fatigue5
- Negative moods: Anger, hostility, depression, confusion, tension, lack of vigor and happiness6, etc.
The solution to cure this syndrome is to go back to a fully consistent monophasic sleep pattern until homeostasis is balance. Usually this takes 1-2 weeks, but this duration can be more or less depending on the amount of sleep deprivation. Before attempting to adapt to a polyphasic schedule again, see Recovery.
Therefore, it is very important to sleep at the scheduled times as precisely as possible! Do not slip in extra naps, extend the core, or skip sleep, to the best of your ability.
Strictness of Sleep Times
After deciding on sleep times of a new polyphasic schedule, you should stick with these sleep times as doggedly as possible. Since the body does not distinguish between weekdays and weekends, the same schedule should be consistent all week. It is also important that you follow the scheduled sleep times as closely as possible each day.
Despite the rigidity, non-reducing schedules have more leeway in scheduling sleep times.
Daylight Saving Time Experiment
We are currently investigating the degree of rigidity in sleep times. However, during fall 2018 and spring 2019, the community has conducted tests Daylight Saving Time (DST) shifts to monitor how fast schedules can be shifted each day. Moreover, we also wanted to see how much it would affect the physical and mental well-being of people.
Results & Recommendations
DST shifts as short as 5 minutes have caused negative effects for most participants. While this does not give conclusive evidence that would delay personal adaptations, it still advocates for sticking to the sleep times as tightly as possible.
The current community recommendation is to not move the alarm times at all, but go to sleep later if absolutely necessary. This teaches you to prioritize your sleep schedule, and to work your life around the fixed sleep times. The new habits will foster sufficient discipline for the later adaptation stages.
Another benefit of keeping the alarm times constant is that several pre-set alarms can stack long before the scheduled sleep times. This setup would eliminate the excuse that the alarm setup causes oversleeping.
Skipping sleep versus moving sleep
As usual, you should stick to your sleep times as religiously as possible for a few weeks to adapt (at least to a reducing schedule). You will also need to go to bed at the same time everyday and avoid as much oversleeping as possible. However, some small mess-ups should still be tolerable. In addition, you really should avoid altering the scheduled sleep time if possible. This is because each permanent change of sleep times will initially bring out the same effects as oversleeping does.
Mechanics of skipping sleep
If you know that you are going to miss some sleep, it is best to skip rather than to move it. Here are certain reasons and mechanics as to why.
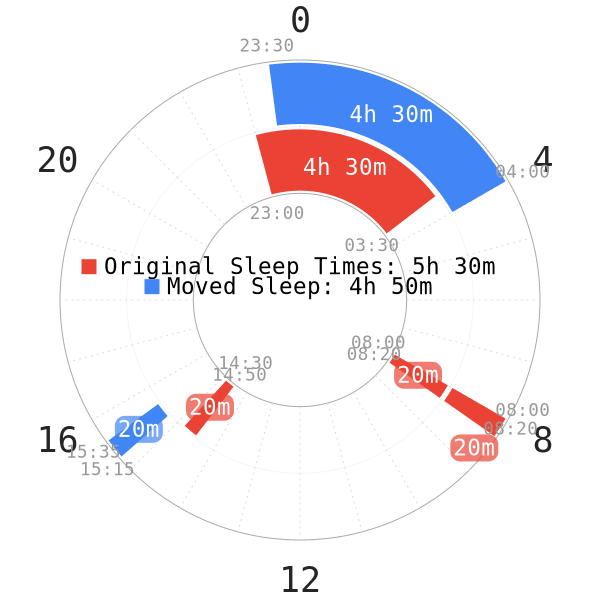
Moving sleep during adaptation (not to be confused with flexing sleep) counts as oversleeping, which pushes adaptation progress back. This is because repartitioning requires strict entrainment of sleep times. In reality, moving sleep has caused the same negative effects as oversleeping.
Missing some sleep, or undersleeping, is not as detrimental as oversleeping. Undersleeping refers to natural wakes from a sleep block because of any reasons. Aside from that, any reason that causes the sleep duration to be shorter than scheduled (e.g, starting a core later) counts as an undersleep.

- While it sets the adaptation back after stage 3, undersleeping does not confuse the body and the entrainment of the schedule the same degree as oversleeping.
- If you actively sleep at later hours than scheduled for a core sleep and still wake up at the scheduled time, you may feel more groggy than usual. This is owing to the misalignment of the sleep cycle, causing the it to end in the wrong sleep stage.
- At first, undersleeping may decrease the feeling of tiredness at the usual sleeping times for a few days after the missed sleep. However, more tiredness dips will occur during the day. Thus, of these two options, undersleeping is almost exclusively the superior option.
- However, losing a nap may increase oversleeping risks later on, so be prepared.
- Set up extra alarms
- Alternatively, ask someone to check on you to make sure you are awake.
- You also must not compensate for undersleeping during the adaptation. Carry on with the adaptation and do not make up for lost sleep. Doing so will count as an oversleep.
Exception
However, there is one exception where moving sleep yields a better result than skipping sleep.
- If you know that skipping sleep will result in an even longer oversleep later, it may be possible to get some sleep before then. This may be a last-ditched effort on a more challenging schedule (e.g, E3), but potentially better than a looming oversleep.
- Make sure the moved sleep block is not too close to the next nap or core. Try to leave at least 3-4 hours before the next sleep.
- If you skip some parts of a core, skip it in chunks of 90 minutes (full cycles) instead. This helps to avoid waking up in the middle of a cycle, or even an SWS wake.
- If you have to skip your whole core, try to at least rake in some naps in during that period of time.
Overall, if you are interested in the idea of flexing your sleep, our article about Flexible Sleep Timing will give you a detailed answer.
Main author: Crimson
Page last updated: 1 April 2021
Reference
- Shoenfeld N, O’Donnell T, Bush H, Mackey W, Callow A. The management of early in situ saphenous vein bypass occlusions. Arch Surg. 1987;122(8):871-875. [PubMed]
- Felkel H, Feuereisl R, Tománek A, Janour Z, Mazur O. [The determination of the type of flow in the trachea and the bronchoscopically accessible bronchial tree]. Pneumonologie. 1971;146(2):120-125. [PubMed]
- Matsunaga H, Nishimoto I, Kojima I, Yamashita N, Kurokawa K, Ogata E. Activation of a calcium-permeable cation channel by insulin-like growth factor II in BALB/c 3T3 cells. Am J Physiol. 1988;255(4 Pt 1):C442-6. [PubMed]
- Blau J. Sleep deprivation headache. Cephalalgia. 1990;10(4):157-160. [PubMed]
- Baehr W, Zhang Y, Joseph T, et al. Mapping antigenic domains expressed by Chlamydia trachomatis major outer membrane protein genes. Proc Natl Acad Sci U S A. 1988;85(11):4000-4004. [PubMed]
- Davis H, Gascho C, Kiernan J. The skin in magnesium-deficient rats. Arch Dermatol Res. 1975;254(1):1-13. [PubMed]
